How the Breast Reduction Surgery is Performed
Breast reduction surgery usually takes about 1½ to 3 hours to perform depending upon the technique, degree of ptosis (sag), and the skill of the surgeon. Your surgery may take longer if other procedures are being performed, such as a breast reduction and lift , abdominoplasty or non breast-related procedures.
Breast Reduction Surgical Markings
|
Your breasts will be marked for surgery to indicate where the incisions will be, identify the center of the sternum, etc. These markings are made with a permanent Sharpie-type marker specifically designed for surgical use. Some surgeons draw your markings in the examination room, some in the O.R. and still others on the operating room table. |
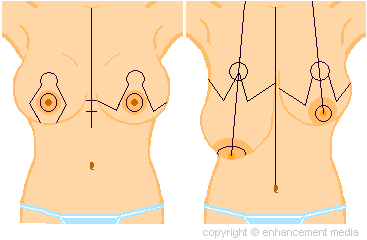 |
There are many variations, so the markings to the right may appear different than your own. The markings will remain on the skin after you are scrubbed with Betadine solution.
IV Insertion
You may or may not have already been hooked up to the saline IV drip while waiting for the O.R. to be prepared for your breast reduction procedure. Other surgeons wheel you into the O.R. and insert your IV then. If you had been given an oral sedative or Valium prior to your procedure, you usually could care less what they are sticking in you. If you haven't been given a sedative, the initial first few minutes until you are anesthetized may be stressful.
Having an IV inserted is similar to having blood drawn. The initial placement of the IV catheter may sting a bit. Catheters are usually placed in the crook of the elbow or back of the hand, depending on your veins.
After the needle is inserted into the vein, it is pulled out and the catheter, a little tube, is left in your vein. Let's call the access system a 'catheter hub' for simplicity. This hub usually contains the catheter, a needle, a flashback chamber and tubing connected with a luer lock. The hub acts as an injection port and is taped to your skin to keep it from getting knocked out. Medications can be injected into the body via this port or be connected the tubing to allow automatic infusion of drugs and intravenous fluids with a computerized drip system. In short, the IV is for a saline drip to keep you hydrated and also acts as a vascular doorway for medications, many times including anesthesia.
You may or may not receive some medications to help you relax or feel sleepy at this time. This can help with pre-operative anxiety if you were not given an oral medication to do so.
Monitoring Equipment
Regardless of the order and manner in which they insert your IV, after you are placed on the operating table they will talk to you for a minute or two and hook you up to the heart monitoring and oximeter machines, possibly wrapping your legs with compression cuffs and other final preparations. Your vital signs will be monitored, including your blood pressure, body temperature, pulse rate/heart beat, and your breathing rate -- all very important factors to determine if you are okay while under anesthesia. The O.R. staff will also check your blood pressure. You have more than likely had your blood pressure taken before with the use of a cuff, which inflates firmly around your arm. You will also have an oximeter clip (or strip) placed on either your finger, your earlobe, or possibly on your big toe. The oximeter machine monitors the oxygen/carbon dioxide saturation in your blood -- this is very important.
You may also have intermittent pneumatic compression sleeves placed on your legs to decrease the risk of Deep Venous Thrombosis (DVT) and subsequent pulmonary thromboembolism. Heavier patients may especially benefit from this. These devices are inflatable sleeves for your legs which are either thigh high or knee high that inflate and deflate to keep circulation optimal. You may also have heat lamps or heated blankets, depending upon the surgeon, your temperature, etc. Your vital statistics must be determined as stable before going any further.
Anesthesia Types Used In Breast Reduction Surgery
If you and your surgeon have chosen an IV liquid sedative, they will either manually insert medications with a hypodermic into a Y site or injection port along the length of the silicone tubing connected to your catheter hub/IV, or your anesthesiologist will attach a bag of anesthetic or use a computer-controlled drip system. The computer system automatically infuses a few drops of anesthetic every few seconds into a drip chamber where it mixes with the saline. The drip crate can also be controlled via the roller clamp. Flow regulators can also regulate the flow rate.
When the anesthesiologist releases the roller clamp, the mixture starts heading towards your body. The effects of the anesthesia are felt soon after injection or opening the roller clamp -- a few seconds in fact. It feels like heat going into you veins then creeping up your arm; then it jumps from your shoulder to a metallic-like taste under your tongue and then you are blissfully anesthetized.
If you have chosen gaseous-state anesthesia (twilight, gaseous general), your mouth and nose will be covered with a mask and you will usually be told to count back from 100. You will usually remember getting only to about 96 before falling fast asleep. Then, the anesthesiologist will more than likely intubate you. Intubation usually involves an endotracheal tube down your throat to deliver gaseous anesthesia to your lungs. However, some surgeons give you a little IV sedation and then intubate you and switch over to gaseous sedation. Both of these maneuvers eliminate the horrible experience of having a tube shoved down your throat while you are awake.
Another option is with the use of a laryngeal mask airway (or LMA). This is a lot like the older intubation for a general, but there is a shorter tube and a little balloon the size of your two thumbs at the end. The tube holds your tongue down and of the way so it does not obstruct your breathing and the balloon inflates and blocks fluid from entering your windpipe, either from saliva or stomach acid and makes a seal so the gas can be delivered to your lungs. It is basically like a diaphragm for your windpipe. You may wake up with a raw throat with either but it is usually less so with the LMA. You may wake up with an irrigated and dry throat regardless because canned or cylinder air is d-r-y. There is no moisture in these tanks. It is your turbinate structure (three little fleshy flaps in your sinuses) inside your nasal structure that mostly warms and humidifies the air you breathe. When you have to humidify your air, your body needs more moisture. The saline drip will assist in this as well.
Another option is with silicone tubing, which is placed in the nose; however this is rarely used as surgeons and anesthesiologists prefer that the windpipe be protected and the tongue firmly held down. Be sure to ask your surgeon which method he will be using if you are interested. Regardless of which method, the gaseous anesthetic is mixed with oxygen and this is how you will breathe during your surgery.
 Sterilizing The Surgical Field
Sterilizing The Surgical Field
The O.R. staff will then scrub your torso (and other areas if you are having other procedures) with a Betadine surgical scrub. The O.R. staff will then rinse off the area with sterile gauze soaked in saline and then repaint your surgical area with a stronger Betadine solution. This will sterilize the area by killing surface bacteria, fungi, protozoa, viruses and yeasts. A common bacteria found on the skin is the naturally occurring Staphylococcus aureus, or simply staph) and decrease your risks of an infection.
Breast Reduction Techniques
There are several breast reduction techniques and these are highly dependent upon your needs as a patient and the surgeon's preference or training.
Some surgeons will use a pedicle, or pedicle flap, to decrease your chances of nipple loss. A pedicle is a flap which is left attached to the original site by a narrow base of tissue to provide a blood supply during grafting.
Pedicle methods include:
-
The horizontal pedicle method, where the nipple is kept on a horizontal pedicle.
-
The lateralizing, or B method, where the nipple is kept on an oblique pedicle.
-
The periareolar method, where the nipple is kept on a central pedicle.
